
Reviewed & Fact-Checked by
Dr. Chyrle Bonk
Veterinarian (DVM)
Learn more about our Veterinary Review Board »
Canine Immune- Mediated Hemolytic Anemia - more commonly known as IMHA - is a relatively rare but complex, and potentially life-threatening disorder of the blood. It can affect humans, cats and dogs.
While it is not common, because it is a serious, chronic disorder it is something that every pet parent should at least be aware of.
What is Canine Immune- Mediated Hemolytic Anemia?
IMHA is a disease of the immune system in which it creates antibodies to the body's own red blood cells and destroys them. In most cases, the reason behind this is never known. The result of this is severe anemia or lower than normal number of red blood cells.

Every tissue in the body relies on red blood cells to deliver oxygen to them. This means that with anemia, there may not be enough carrying capacity and tissues may starve and die.
- Dr. Chyrle Bonk, DVM -
Severe anemia can be life-threatening, so immediate treatment is a must.
What Causes IMHA in Dogs?
IMHA occurs when the body’s immune system destroys red blood cells
There can be a number of reasons that a pup - even a young, previously healthy pup - can develop IMHA. To complicate things even further there are two different types of IMHA: primary and secondary.
Primary IMHA, which is the most commonly diagnosed form, has no known cause, but is believed to be genetic in nature.
Secondary IMHA is the 'side effect' of another health condition. This can be a vaccination reaction, cancer, exposure to toxins, Lyme disease, infections or a bad reaction to medications.
There are also two different ways IMHA can present itself.
Intravascular IMHA means that red blood cells are destroyed throughout the bloodstream, while in extravascular IMHA they are destroyed within the liver and spleen.
Both forms CAN be extremely dangerous if left untreated.
Are Some Breeds More Likely to Develop Immune- Mediated Hemolytic Anemia?

Sadly Cocker spaniels are the poster dog for IMHA
Secondary IMHA can affect any pet dog, BUT primary IMHA is believed to have a genetic component that is found more frequently in some breeds than others.
These breeds include:
- Cocker Spaniels
- Springer spaniels
- Dachshunds
- Irish setters
- Standard poodles
- Bichon Frises
Research has also shown that middle-aged to older pets and females are somewhat more likely to develop IMHA, but no one is quite sure why that is.
How can I tell if my dog has IMHA?
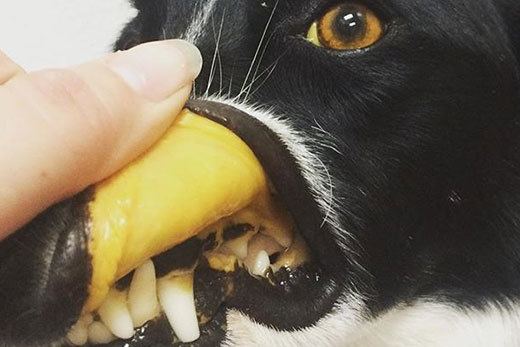
Check the color of the eyes and gums to look for jaundice or icterus in IMHA, like in this dog
IMHA can be hard to pinpoint - for pet parents at least - but as it is a severe form of anemia, there are some telltale signs. They include the following:
- Lethargy, either after normal exercise or in general
- A sudden loss of appetite or refusal to eat
- Weakness or collapse
- Discolored urine (dark red or brown)
- Vomiting
- Faster heart rate
- Pale or yellowed (jaundiced) gums and eyes.
Many of these symptoms are also related to other conditions, so they do not indicate for sure if your pup is suffering from IMHA. Time is essential, so if you see any of these signs, don't delay seeing your vet.
DVM Tony Johnson, has this stark message to say about how serious you should take any of these signs of IMHA in your pet dog:

It can happen with remarkable speed – one day your dog is happily snoozing by the fire, the next day your veterinarian is telling you that he’s in a 50:50 battle for his life.
If at all in doubt, err on the side of caution and get your pup to the vet as soon as possible, especially as secondary IMHA is usually a sign of another health condition as well.
How is Canine Immune- Mediated Hemolytic Anemia in Dogs Diagnosed?

A vet will perform a standard blood test if anemia is suspected
The first thing a veterinarian will do is determine if a dog is anemic by performing a simple blood test. By measuring the packed cell volume, the vet will be able to diagnose anemia. They will then need to track down the cause of that anemia by running further tests.
Your vet will need to investigate every possibility. This investigation should include an extensive history and thorough diagnostic testing. Bloodwork to check organ function and diagnose infections and a urinalysis should be performed. Ultrasound scans and x-rays will also be used to rule out conditions like cancer, and to look for any organ damage that the disease may already have caused.
According to Dr. Christopher G. Byers, "one common mistake practitioners can make is not being aggressive enough in identifying any underlying causes, such as neoplasia, that may make the IMHA a secondary disease".
What are the Treatment Options for IMHA in Dogs?
Intensive care hospitalization with red blood cell transfusions may be necessary
The treatment a pet dog receives for IMHA will vary according to its severity, whether it is primary or secondary and whether or not another health condition needs to be treated as well.
In most cases, the first treatment administered will be a blood transfusion so that the pup's red blood cell supply can be quickly replenished. From there, the cause of IMHA will be looked into.
If it is determined to be a primary condition, your vet will look at beginning long term immunosuppression, using high doses of steroid medications. This will help prevent the body from attacking the new red blood cells that have been introduced via blood transfusion and the new red blood cells that the body produces.
If the IMHA is determined to be a secondary health condition, then the underlying health condition will have to be treated as well. This may include antibiotics, surgery, or toxin antedotes.
To summarize, when looking at IMHA treatment there are three main goals the therapy should achieve:
- Increase the packed cell volume with a blood transfusion.
- Address the underlying cause, if any, for the IMHA.
- Suppress the immune system to stop its attack on the red blood cells.
Medication
Dogs that receive treatment are on medication for several months. Steroids like prednisone are the cornerstone of immunosuppresive therapy.
Additional immunosuppressive drugs, antibiotics, and anticoagulant drugs include: cyclosporine, famotidine, melatonin, doxycycline and aspirin are the typical initial treatment regimen for dogs with confirmed IMHA in which no underlying primary disease is found (idiopathic IMHA).
Prevention and Recovery

Avoid walking your pup in long grass and check for ticks
The prognosis for dogs diagnosed with IMHA varies significantly. If the episode was secondary, managing the underlying cause can increase their survival odds significantly.
If the IMHA is primary, the pup will need to be on immunosuppressive drugs long-term, and some will need them for the rest of their lives. Long-term immunosuppresion has many side effects, including an increased chance of contracting infections and decreased healing abilities.
For dogs that respond quickly to immunosuppressive therapy and do not require repeated blood transfusions, the prognosis can be good.
Follow-up care generally includes repeat labwork and physical exams.
Sadly, many dogs can experience a relapse at some point in their lives, usually when medications are discontinued or tapered.
Because the real cause of primary IMHA is not really understood there is really nothing that can be done to prevent it, other than to ensure your younger dog gets his vaccinations early on.
The good news is that there have been a number of recent research breakthroughs and veterinary medicine for IMHA is improving every day.
In the case of secondary IMHA, some of the possible causes can be prevented to a certain extent. Try to keep your pet away from toxins, including household chemicals, and, to help minimize the risk of Lyme disease by routinely checking for ticks, especially if you live in the Northeastern United States.
Knowing the early signs of IMHA is also your dog’s best chance at survival. The early a dog gets diagnosed and treated, the better the outcome.





We adopted Sammie from a shelter when she was just one month old ( Dec-2017 ) and it was LOVE at first sight. It felt like she chose us as much as we chose her. She was such a tiny little puppy and we had no way of knowing she would grow to be this beautiful big wolf.